Q Exchange
Using the Patient Activation Measure for a patient-centred TIA service
- Idea
- 2018

TIA Background:
There are approximately 46,000 are first time Transient Ischemic Attack (TIA) incidents in the UK every year. TIA causes a brief episode of neurological impairment, due to a loss of blood flow in the brain. TIA is a warning sign, 17% of people will go on to have a full stroke within 3 months, and the risk of further vascular event (cardiac or stroke) remains elevated for at least 10 years. Worryingly, the rate of stroke in people aged 45 and over is expected to rise by 59% in the next 20 years. If we are serious about reducing the incidence of stroke, then we must be serious about supporting people with TIA to proactively manage their risk factors.
Secondary prevention (modifying risk factors via medications, monitoring and lifestyle changes) post TIA is known to reduce risk of future vascular events; improving outcomes for individuals, reducing burden on Stroke services, wider NHS resources, and reducing the impact of Stroke on wider society.
Current models of care:
Research has offered a blueprint for national standardisation of acute phase TIA support (rapid assessment within 24 hours, investigations and treatment). In contrast, follow up post TIA is varied, but typically involves seeing a healthcare professional at one month post event.
Across Dorset variability of follow up provision reflects resource availability within individual teams, rather than patient needs. Each site offers a “one size fits all” model of care. This project was prompted by regional service reconfiguration (Dorset One Acute Network/Vanguard) facilitating collaboration to improve quality of provision across Dorset for all.
Follow up aims to provide health and well-being guidance supporting individuals to make changes to reduce risk of further vascular events. National guidelines outline ‘what’ to do to optimise secondary prevention (medications, clinical parameters for management of risk factors, lifestyle changes), however it offers little direction on ‘how’ best to enable individuals to implement and sustain these behaviours. Adherence to recommended secondary prevention medications is an acknowledged challenge, with adherence as low as 35% – demonstrating missed opportunities to reduce stroke risk.
National guidance recommends ‘tailoring’ support to meet needs of individuals. Without a reliable structure to measure individual’s capability to self-manage and assessing risk related to this, ‘tailoring’ education and support is not meaningfully achievable.
How could PAM help?
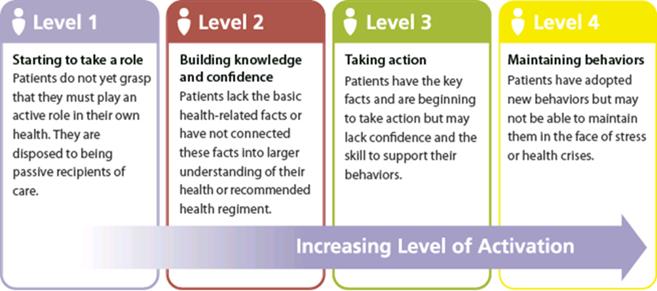
NHS England endorses PAM as a core-enabler of supported self-care. PAM is a licensed tool to assess an individual’s knowledge, skills and confidence to self-manage their health and healthcare. Responses to a questionnaire are quantified resulting in an activation score (grouped into four levels).
Higher level activation is associated with improved patient experience, improved clinical outcomes, increased ability to sustain healthy behaviours and reduction in emergency services usage. Activation is not static; evidence showing benefits of responding to activation to better health outcomes is growing.
Project aims
Using an experience-based-co-design approach we will seek to redesign TIA follow up services in Bournemouth and share this learning with colleagues across the regional clinical network. PAM will be integrated within ‘live’ clinic based co-design, encouraging inclusive, ‘whole-population’ engagement that allows co-design to be representative of the range of service users. Responses will be grouped by activation level to allow understanding of different needs/opinions.
Working with patients and wider stakeholders we will design future pathways of care that reflect and respond to their differing activation needs. Our aim is to better enable self-management to effectively reduce risk of future vascular events in the months and years that follow discharge from TIA services. Our project will consider system-wide use of resources and wider community pathways beyond the TIA service’s current reach (health coaching, behavior change specialists, development of peer support networks), better integrating our patients and our service within the Dorset community.
Our approach is novel; there is no published data using PAM post TIA. There have been benefits demonstrated within wider cardiovascular disease pathways. This bid is to provide the resources to design and implement the new pathways. We envisage the new pathway to incorporate integration across health and social care sectors, to maximise expertise and resources across the system.
Who is involved?
Our well-established steering group has a proven record of successful quality improvement initiatives demonstrating commitment to the development of self-management support and learning across the region (previous projects have included Patient Activation projects within Diabetes and COPD services and the development of regional Rehabilitation, Reablement and Recovery Quality Guidance).
The steering group includes representatives from across the Wessex region:
· Clinicians
· System Leaders
· Commissioners
· Voluntary Sector
· Wessex Clinical Network
We are working in collaboration with:
· Dorset One Acute Network
· Patient Engagement teams
· Dorset CCG (providing PAM licences)
· Wider support services/stakeholders (e.g. Dorset based Health Coaching)
· Local Quality Improvement teams
How you can contribute
- Support in pathway redesign
- Working with patient and public to ensure partnership working is achieved.
- Guidance in experience-based co-design processesGuidance to support working and influencing across organisation boundaries.
- Guidance on measuring change in ways that our meaningful to patients and services
- Learning from others within the Q community and sharing our learning with colleagues undertaking similar QI init
Comments
Dr Suzanne Ragab, Trust Lead Clinician for Clinical Audit 20 Jun 2018
This is an excellent Quality Improvement Project which aims to put patients individual needs at the centre of their care whilst ensuring that NHS resources are used to their maximum impact to affect health behavior change.
Morwenna Gower 19 Jun 2018
Fantastic project which will help to demonstrate impact of creating services which recognise the need to support behaviour change and deliver individually tailored care. I am in full support of this project! Good luck!
Alison Shave 19 Jun 2018
A great opportunity to shape services to better meet individuals needs and enable/ support behavior change for a healthier future!
Michelle Dharmasiri 15 Jun 2018
Great project. A fantastic opportunity to provide evidence to support more tailored follow-up for a large group of NHS patients.
Carl Adams 15 Jun 2018
Thank you for your support.
Jane Williams 7 Jun 2018
The opportunity to continue to contribute to the growing evidence base about the importance of supporting health behaviour change in both our services users and staff is of paramount importance. Testing across a range of conditions and settings will help commissioners to understand where real impact can be made and support implementation of contemporary models of care which include activation and health behaviour change.
I completely support this project.
Comments are now closed for this post.