Rapid innovation and learning have been at the heart of our immediate response to coronavirus (COVID-19). We have been hosting a series of workshops to support Q members and others to develop how they capture the learning and innovations that are taking place.
This is a write-up from our third workshop in the series, which explored practical ways to navigate the uncertainties from the COVID-19 pandemic, with ideas to help teams develop a clear vision for the future.
This page includes:
- An introduction to futures and foresight
- Practical tools and models from futures and foresight
- Themes from breakout discussions that explored current problems and future possibilities
Want to find out more?
- Download the full write up
- Sign up for our fourth workshop in this series
- Join the conversation on Twitter via #RapidQI
What do we mean by futures and foresight?
Futures and foresight methodologies encourage and support us to think about and plan strategically for the future. They are less about predicting the future, and more about looking for actions that can be taken now to shape what comes next, with the knowledge that the future is not predetermined. Futures and foresight tools can be used to help us make sense of the present; to identify trends, map alternative futures and come up with plans for how to reach the future that we want.
Futures and health care
Futures methodologies can be particularly useful in health care, as many of the models acknowledge the complexity that exists in systems. While futures theory is used most in policy or academia, there are many tools and methods that have been developed or adapted for teams and organisations as part of planning and strategy development. Find out more about the Health Foundation’s Shaping Health Futures programme.
Futures and foresight tools
The generic foresight process from Joseph Voros shows clearly the phases you need to move between, and in particular the questions that need to be explored at each of the four stages of the model.
Another tool is the Three Horizons model by Bill Sharpe at International Futures Forum. It is a visual model that can work well for group discussions.
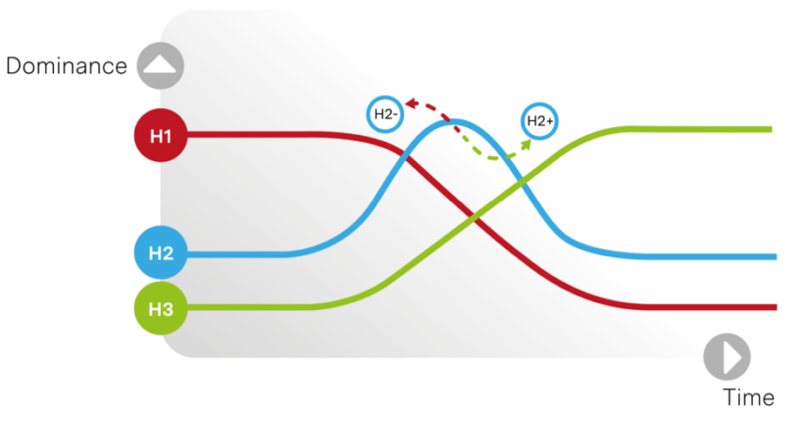
The model looks at dominance and time, showing that in most scenarios there is a dominant way of doing things right now (H1), which will be replaced by a completely different way of doing things (H3). Changes and innovations that take place between them can both speed up and slow down this change (H2).
In the workshop, we had a deeper look into the Three Horizons model, with a case study from Public Health Wales showing how it can be used in teams. Details are included in the full write up.
The activity provides space to think about things that are uncertain in your environment, then helps prioritise what is most critical and most uncertain
If you would like to think about how your team can be better prepared to act, and respond to, disruptions, try the Liberating Structures activity Critical Uncertainties. The activity provides space to think about things that are uncertain in your environment, then helps prioritise what is most critical and most uncertain and come up with scenarios for how this can happen. Looking across the different scenarios can help to identify actions you can be thinking about now to help in multiple future scenarios.
Teams could also look at scenario planning using the 4Ps. This model helps identifying potential futures by discussing which of them are possible, plausible, probable and preferable. Further detail can be viewed in the full write up.
An exploration of current problems and future possibilities
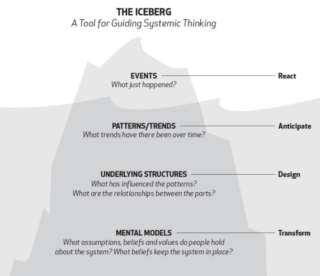
The breakout sessions followed the Iceberg model – a tool for guiding systematic thinking. This helped participants think about the systemic issues causing the problems they are seeing, and where they need to be looking for innovation and change to take place.
From discussions in breakout groups it emerged that, looking to the future, people wanted to see:
Greater service user input in service design/changes
Participants recognised the lack of engagement with service users during the pandemic and discussed the importance of bringing in these voices as services transform.
Continued focus on service changes, particularly video consultations
There are high hopes for making video consultations sustainable going forward. There was acknowledgement of the need to be aware of introducing a new set of inequalities, with strong feelings about the need to explore different options for patient interaction. There is radical potential for this to unlock how services could be organised in the future (e.g. to access interpreters, to pool capacity) that could be transformational.
More joined up working, leading to more collaboration and less fear
Participants wanted to see health and social care truly collaborating, with joined up planning across the system and people volunteering to help areas outside of their normal job description.
More staff involvement to make changes happen, and less organisational hierarchy
There was a sense of wanting to keep the team approach and team autonomy that came to the forefront during the pandemic, with less top down imposition, and more voices in the room where decisions are made.
Read a summary of the emerging themes and discussions in the full write up.