Q Exchange
Pop-up resources for innovative real time delirium and dementia education
- Idea
- 2018
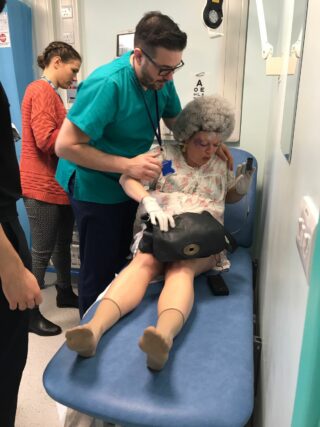
Meet the team: Innovations in Delirium Education
Also:
- Dr Rachel O’Toole, Consultant Physician in General Medicine & Care of the Older Person
- Clinical lead for dementia and delirium
- Julie Vale, Acute Care of the Elderly Practitioner
- Karen Bird, Acute Care of the Elderly Practitioner
- Carol Mayl, Acute Care of the Elderly Practitioner
- Joan Allen, Acute Care of the Elderly Practitioner
- Dr Ella Sherman, ST4 Care of the Elderly
Delirium is a common and serious condition, often under-recognised in both the acute hospital trust and the wider community. Patients with delirium have an increased risk of poor outcomes with associated increases in health and social care needs that can impact individuals and their carers. This has significant cost implications for organisations involved in their care. It is therefore critical that staff across the health and social care system who come into contact with people with delirium are confident in recognising the condition and in caring for people with delirium and have the necessary skills to ensure prompt and personalised care and treatment.
Delirium detection and management needed improvement at Musgrove Park Hospital in Somerset. A new cognitive screening pathway was therefore introduced on the Acute Medical Unit (AMU) to improve detection of delirium. Weekly audits of a representative patient sample on AMU show that we are now achieving screening in 80% of patients over the age of 65 years on admission, from a rate of less than 50% at the start. As part of implementing the hospital- wide pathway, a delirium educational programme for all staff is essential. This is the next stage in our improvement pathway for people with cognitive impairment.
Simulation has been shown to be a cost-effective and enjoyable educational tool. We have successfully trialled a ‘pop-up’ simulation based training model for delirium and dementia in the Emergency Department and AMU. It has been phenomenally successful and we are now asking you for money to help develop this further so that it can be used on a much larger scale by other trusts and organisations across the UK health and social care system.
Our pop-up model is incredibly flexible, adaptable and replicable. It is quick to set up and run and consists of a real time simulation of an older person experiencing delirium. It includes background information and ambulance documentation about the person, and requires a set of props (which are listed) to make it faithful and credible. It requires someone with knowledge of caring for people experiencing delirium or a trained actor. Staff are placed into the simulation but others can observe. The simulation allows staff to practice their approach, diagnostic and care skills and improve their self confidence in detecting, treating and managing people with delirium. The de-brief is a critical component of the model to ensure learning outcomes are achieved. All staff who have undergone this innovative training have provided consistently excellent feedback. People living with dementia are at very high risk of developing delirium but also require a careful approach to management and education in how to de-escalate situations. This model can be extended to provide teaching scenarios for dementia as well as delirium.
Investment would allow us to:
o Create a package that other trusts and organisations can use to run ‘pop-up’ training with minimal effort and cost in their own organisations
o Provide supporting training materials, for example videos and on-line resources and applications that can be used to support simulation training, for inductions or as an alternative where a simulation is not possible
o Extend this model into training for dementia as well as delirium
o Potentially extend this model to the wider community for training in care homes and GP surgeries
How you can contribute
- People with delirium experience to be simulation ‘patients’
- Input into and peer review of simulation and training materials
- Writing of scenarios and ensuring educational needs are met
- Regular review of the model ensuring alignment with local and national guidelines
- Help to build relationships with other organisations interested in running this training
Further information
SIM feedback and AMU graph (PDF, 230KB)
Comments
Andrea Gibbons 20 Jun 2018
I've had the privilege of discussing this bid with the team working on it, and it's really exciting and effective. I truly hope that they get the chance to make their project a reality. Good luck!
Marie Little 20 Jun 2018
I agree with Claire and it is great to see this progressing further.
Claire White 20 Jun 2018
I've heard all about this from attendees at some of the early sessions that you have run, and the feedback was amazing. They were so enthusiastic. It would be great to roll this out further and professionalise it so that other trusts can benefit from it too. Good luck!
Comments are now closed for this post.