One of the biggest challenges facing the NHS after the COVID-19 pandemic is the length of time people are waiting for treatment. The Patient Experience Library has launched a new tool using data sourced from NHS England. Any NHS patient or staff member can look up waiting times for treatment at their local hospital and can compare this across up to ten trusts in a single search. This introduces a new level of visibility and insight into the capacity and performance of the NHS through a free, user-friendly tool.
What we found is that being on a waiting list is fundamental to people’s perceptions of quality of care
According to Ipsos Mori, half the population see ‘improving waiting times for routine operations’ as the top priority in health care. Last year, The Patient Experience Library worked with National Voices and Care Opinion on a report that looked more deeply into the experience of patients waiting for care. What we found is that being on a waiting list is fundamental to people’s perceptions of quality of care, and it has a considerable impact on each patient’s quality of life. In this report, people who had been on waiting lists talked about being in an information vacuum for long periods of time. This left them with a feeling of ‘a lack of control’, and an inability to ‘get on with life’. Others described a sense that they were ‘fighting the system.’
Waiting list data is, of course, published on the NHS website. But the data is presented in a way that perfectly matches the Health Foundation’s description of NHS data that is ‘hard to locate online with multiple spreadsheets to choose from and large Excel workbooks to download and navigate’.
Things are not much easier for NHS staff than they are for patients. One of the heads of elective care who works at a large metropolitan NHS trust showed us how staff access this buried data. After downloading an NHS England dataset, she had to unlock a series of hidden worksheets within an Excel spreadsheet and then spend hours manually extracting the data that she needed. Even this experienced and senior member of staff felt that there must be a simpler, better way.
Anyone involved in quality improvement knows that the data that has the best chance of being used must be accurate, easy to find, and clearly presented.
This point has been well made by the BMJ, whose Using Data for Improvement guidance says that data should be ‘displayed transparently so that all staff, service users, and patients and families or carers can access them and understand how the service is performing.’
Tired of the monthly struggle to work out what on earth was going on with waiting lists, we decided to do something about it. We asked ourselves whether we could create a dataset that would be up to date, instantly accessible, free to use, and so simple that no training would be required. As it turns out, the answer to this question is yes.
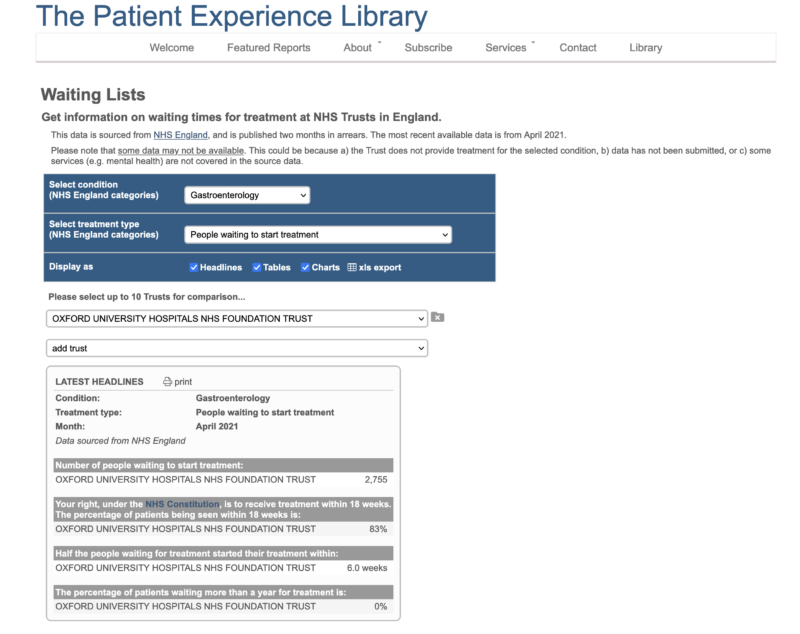
Our waiting list tool takes waiting times for every treatment in every NHS Trust in England and puts them all in one place. It brings this data into the light and enables anyone, at any time, to see NHS waiting times. The data is presented in a table written in plain language, and describes a number of factors including how many people have begun treatment, how many are waiting for treatment and the percentage of people being seen within 18 weeks. It uses graphs to show the number of people who have begun treatment, the median waiting time over 52 weeks, and allows users to make statistical comparisons for up to 10 trusts.
Tools like these can help both patients and professionals to see how trusts are performing on waiting times. They can be built quickly and affordably. They should be a basic part of an NHS looking to integrate services – and integrate quality improvement.
Further reading
The Bedpan: Waiting times, not care inequalities, are the public’s priority post-pandemic – Alastair Mclellan
Patient Noun Adjective: understanding the experience of waiting for care – National Voices publication
Comments
Hurian Anthony De Zilva 28 Jan 2022
Can I view waiting list for my lower back operation
Miles Sibley 28 Jan 2022
Hello Hurian - if you're waiting for a back operation, I'm guessing that your "treatment type" will be "Trauma and Orthopaedic". You might want to check that with your GP though. On the waiting list tracker, you can select the Trust where you'll be getting your treatment, then select "Trauma and Orthopaedic" and you'll see the overall waiting times. We'd like to give people the ability to dig deeper - ideally to see things like how long they personally have been on the waiting list, and how much longer they might have to wait. But for that, we need NHS England to give us access to more of the data, and so far they won't. Hope that helps anyway.
Susan Ford 7 Feb 2022
I have been on waiting list for a knee replacement for well over a year after suffering a knee fracture over 3 years ago. I have rung Barnsley hospital a few times and got answer phone where no one ever answers my question as to where I am on the waiting list
Carole Slack 28 Feb 2022
I had my pre op assessments 5 weeks ago for a knee replacement, the consultant said I will do this priority. Still not heard anything. Its hard when a patient like me cant make any plans for example who will have my dog at short notice. Will I have to cancel other appointments because I dont have a date??
SusanFord 28 Feb 2022
I had a pre assessment for a knee replacement in October and heard nothing since plus no answers from being asked to leave phone messages. I have an untreated knee fracture from 3 years ago and arthritis. It is difficult to get about or plan for anything in case I get an appointment at short notice. Just to have an idea of waiting would be helpful.
Carole Slack 28 Feb 2022
I can understand how you feel I'am the same, he said there was no cartilage left it was bone on bone. I got my pre op three days later now nothing. I am trying to find the new web site the Gov have agreed saying you can look where you are on the list but I can't find it !!!
Miles Sibley 28 Feb 2022
Susan, Carole - Your comments echo so much that other people have said about being on lengthy waiting lists - feeling left in an information vacuum, with your life on hold, etc.
The government's new website is https://www.myplannedcare.nhs.uk/ but it won't tell you anything other than the average waiting time for treatments at your local Trust.
Ours is at www.patientlibrary.net/waitinglists It offers a lot more information, along with Trust-by-Trust comparisons - but we'd still like to go further with it.
One example would be that we could show waiting times for "hip replacement", "knee replacement" etc, rather than just "Orthopaedic". Another would be that we could show how many people are in each of the four patient priority categories. Those sorts of things would help people to get a much better idea of where they actually were on the list.
To make those improvements, we have to work with NHS England, as they have access to the kind of data we need. We have been asking them ever since we launched our waiting list tracker in June 2021. But all they have done is spend all of that time, plus large amounts of taxpayers' money in coming up with My Planned Care, which is a much inferior version of what we are already providing for free.
We'll continue to ask them to work with us, but our concern is that they have now committed to their own version, so might not want to...
Claire Kettle 17 Mar 2022
I’m waiting for a total knee replacement, the NHS cancelled 2 op’s because of covid then I cancelled when the death rates increased. Is there a way i can get an idea of when I could be called as I’m unable to make any plans, I’m on the NHS list for Stepping Hill Hospital, Stockport, Cheshire
Miles Sibley 17 Mar 2022
I'm sorry Claire - we don't have access to personal healthcare records, so you can't use our tracker to find out exactly where you are on the list or how long you might have to wait.
Your situation is similar to so many people's, and we had hoped that NHS England would do something to help people get a better idea of their own personal waiting times. A few weeks ago, Secretary of State Sajid Javid went on the BBC Radio 4 Today programme to announce the launch of a new government website called My Planned Care (https://www.myplannedcare.nhs.uk/)
He said, "For the first time, every patient in England will be able to go on line and see where they are on the waiting list". Unfortunately that's not correct. All My Planned Care offers is one statistic: average waiting times for treatments.
In the meantime, the best I can suggest is that you ask your GP if they can get any information for you. Or you could maybe try the Stepping Hill Hospital Patient and Customer Services department - 0161 419 5678 or email PCS@stockport.nhs.uk Another alternative might be Healthwatch Stockport: https://www.healthwatchstockport.co.uk/contact-us
Lynda Banister 8 Apr 2022
I'm trying to find out how long I really have to wait, (not the vague answer I've been given), for an urgent MRI scan to see if melanoma has spread from the surgical site. There does not appear to be any way of finding out the current situation which I'm sure is unlikely to conform to the standard 2 weeks. Recent experience has made me less than confident that clinicians will/can give me an accurate estimate. Is there anything I can do?
Miles Sibley 11 Apr 2022
I'm sorry Lynda - I'm not really qualified to advise on this, and I also don't know where you are. All I can suggest is that you try contacting your GP, or perhaps the patient support team at the hospital (sometimes called the PALS team, or could be called customer services or patient information and advice).
You could also maybe try your local Healthwatch, who should have a website that you could find via Google. If you have had a letter from the hospital, there might be a phone number for the department where the scans are done, that you could phone. Or, you could maybe try your Clinical Nurse Specialist, if you have one.
I'm aware that you might have already tried all of this, so apologies again if this isn't very helpful.